When you’re in the midst of new motherhood, and something feels deeply wrong, it can be confusing to figure out what you’re actually dealing with. If you have ADHD or suspect you might, there are some critical things your provider may not have told you. So, here’s what you need to know about ADHD and postpartum.
1. ADHD, postpartum depression, and anxiety share so many symptoms that one is often missed.
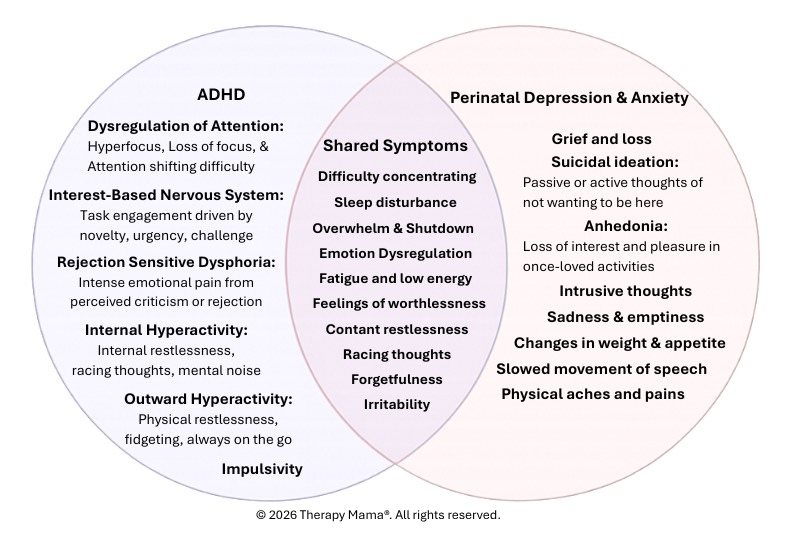
Poor concentration, forgetfulness, emotional dysregulation, overwhelm, irritability, and brain fog show up in both ADHD and postpartum depression and anxiety.
When a new mother walks into a provider’s office reporting these things, the default assumption is postpartum mood and anxiety disorder (PMAD). And that assumption is often correct.
But if ADHD is also part of the picture and no one asks the right questions, it stays invisible.
You can be treated for postpartum depression and anxiety, but if ADHD was never brought up, then you are only receiving partial treatment.
2. Postpartum systematically dismantles the structures and strategies ADHD brains depend on.
ADHD brains rely heavily on structure, routine, sleep, and support for dopamine regulation. This is because the executive function system in an ADHD brain doesn’t operate as automatically or consistently, so it needs more external support to help with things like getting started, staying focused, and following through.
The postpartum period removes structure, routine, sleep, and support for dopamine regulation all at once.
The sleep deprivation alone measurably worsens ADHD symptoms beyond ordinary tiredness. Add the loss of external deadlines, the unpredictability of infant care, and the erosion of whatever coping strategies were holding things together before, and you have a perfect storm that destabilizes an ADHD brain.

This is just neuroscience, not a moral failure.
3. Many women with ADHD aren’t diagnosed until after they have children because postpartum is often the breaking point.
Women with undiagnosed ADHD frequently make it through school and early adulthood by compensating and masking in ways that eventually stop working. They appear to be functioning, sometimes even high-functioning, while spending enormous amounts of energy just keeping up.
The postpartum period burns through those reserves. New motherhood utilizes a lot of executive functioning. What emerges can look like postpartum depression and anxiety, and it may genuinely be those things. But without identifying the ADHD underneath, treatment for a postpartum mood and anxiety disorder alone will only partially help.
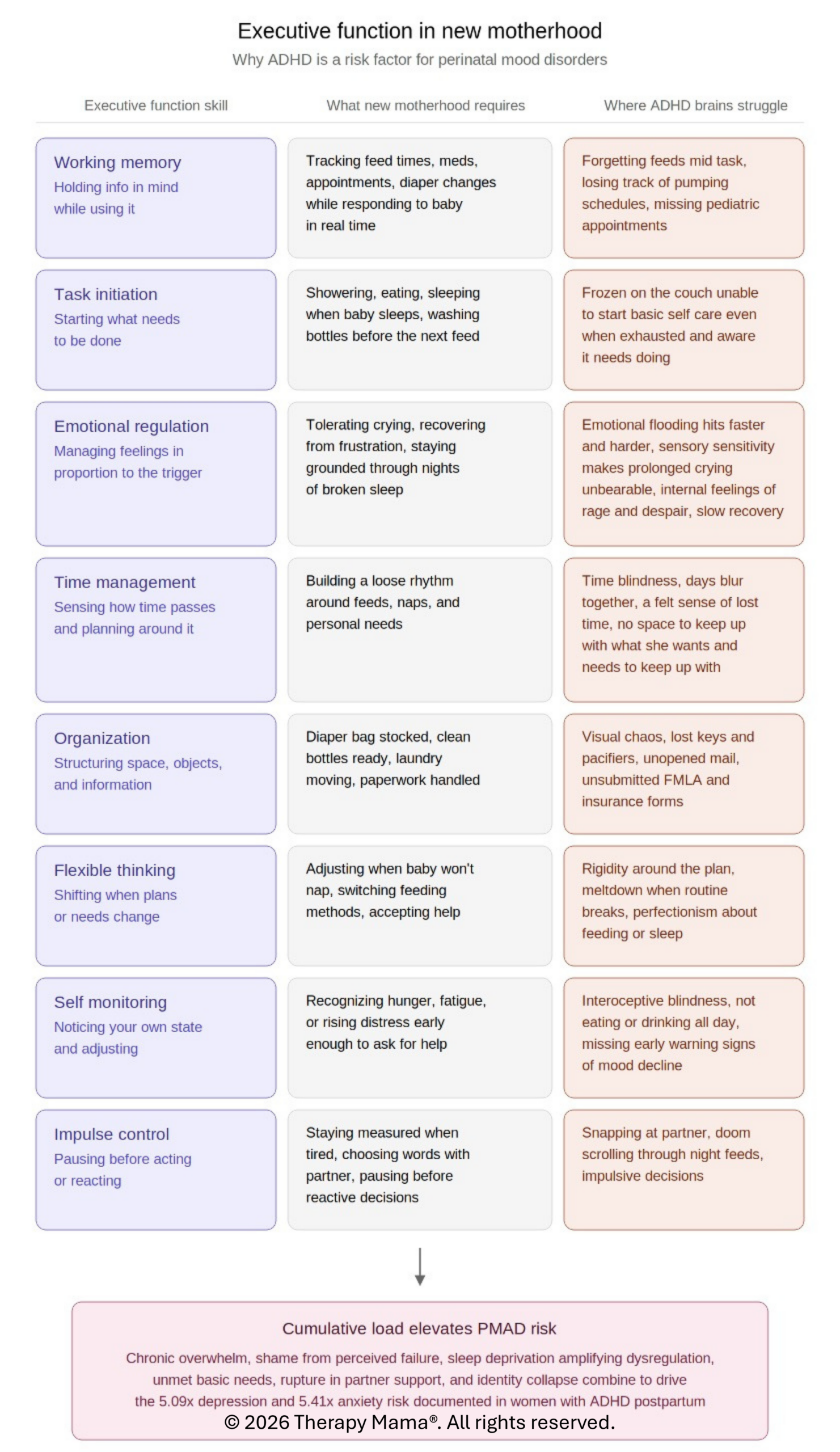
Executive function in new motherhood
The eight executive function domains shown below are the demands every new mother faces in the early postpartum period. When ADHD is in the picture, the same domains that are already a struggle become the places where new motherhood quietly breaks down, and the cumulative load elevates risk for a perinatal mood and anxiety disorder.
4. ADHD is a risk factor for postpartum depression and anxiety.
ADHD is a risk factor because of everything mentioned above. In fact, women with ADHD are 5x more likely to experience postpartum depression and anxiety than women without ADHD.
Women with ADHD are more sensitive to hormonal shifts. Rising estrogen during pregnancy often improves ADHD symptoms, but when estrogen drastically drops after delivery, ADHD symptoms exacerbate.
Estrogen directly influences the brain chemicals that regulate attention, mood, and emotional control, dopamine, norepinephrine, and serotonin. For women with ADHD, this is a big deal.
During pregnancy, rising estrogen gives the ADHD brain a natural boost. This is why many women with ADHD describe pregnancy as a time when they finally felt like themselves. They feel clearer, more focused, and less behind. If you can relate, this is why.
Then the baby comes, and estrogen plummets.
The ADHD symptoms that felt manageable during pregnancy come back. And sometimes harder than before. Serotonin takes a hit too, affecting mood, anxiety, and sleep. Everything postpartum already makes it harder, and everything ADHD already makes it harder.
For a woman living with both, this is not two separate problems. It is one neurological perfect storm.
Other symptoms of ADHD that compound the struggles many moms have include rejection sensitivity, which amplifies mom guilt, racing thoughts that prevent sleep even when the baby is finally down, time blindness, which makes the overwhelm worse, and emotional dysregulation hits faster and harder.
If you have ADHD and postpartum depression or anxiety, you need both to be recognized and both to be treated. Treating only one is like addressing half the problem.
5. You may need to advocate for yourself to get an accurate picture.
Standard postpartum screening does not include ADHD. Providers are not routinely asking whether you struggled with focus and organization before pregnancy, whether you relied heavily on structure that has now disappeared, or whether you’ve always felt like you were working harder than everyone else just to keep up.
That means the burden often falls on you to bring it up. If something still doesn’t feel right after treatment for postpartum mood and anxiety disorder, that is worth revisiting. Ask specifically.
You are not overcomplicating things. You are trying to get an accurate diagnosis and you deserve one.
If you’re reading this and can relate to any of these experiences, you are not alone. And you are not lazy, dramatic, or too much. You may simply be a woman whose brain has never been fully understood, including by the people who were supposed to help you.
Start the conversation. Tell your provider what’s actually happening. Ask the questions this post raised. And if you’ve already been treated and still don’t feel like yourself, keep asking. Something being complex to diagnose doesn’t mean it isn’t real. It means you need someone who will look more closely.
And if you’ve already been treated for postpartum depression or anxiety and still don’t feel like yourself, that is a signal worth following up on.
Getting an accurate picture of what you are experiencing is not asking too much. It is the first step toward actually feeling better. Because your mental well-being matters.
Jacqueline V. Cohen, LPC, ADHD-CCSP, is a licensed therapist who specializes in perinatal mental health and adult ADHD. To learn more about her work, visit her website. You may also contact her by email.
Osianlis, E., Thomas, E. H. X., Jenkins, L. M., & Gurvich, C. (2025). ADHD and sex hormones in females: A systematic review. Journal of Attention Disorders, 29(6), 587–601. https://doi.org/10.1177/10870547251332319
Andersson, A., Garcia-Argibay, M., Viktorin, A., Ghirardi, L., Butwicka, A., Skoglund, C., Bang Madsen, K., D’Onofrio, B. M., Lichtenstein, P., Tuvblad, C., & Larsson, H. (2023). Depression and anxiety disorders during the postpartum period in women diagnosed with attention deficit hyperactivity disorder. Journal of Affective Disorders, 325, 817–823. https://doi.org/10.1016/j.jad.2023.01.069
Get your free copy of my e-book: Motherhood and ADHD
You will also receive a subscription to my newsletter.



